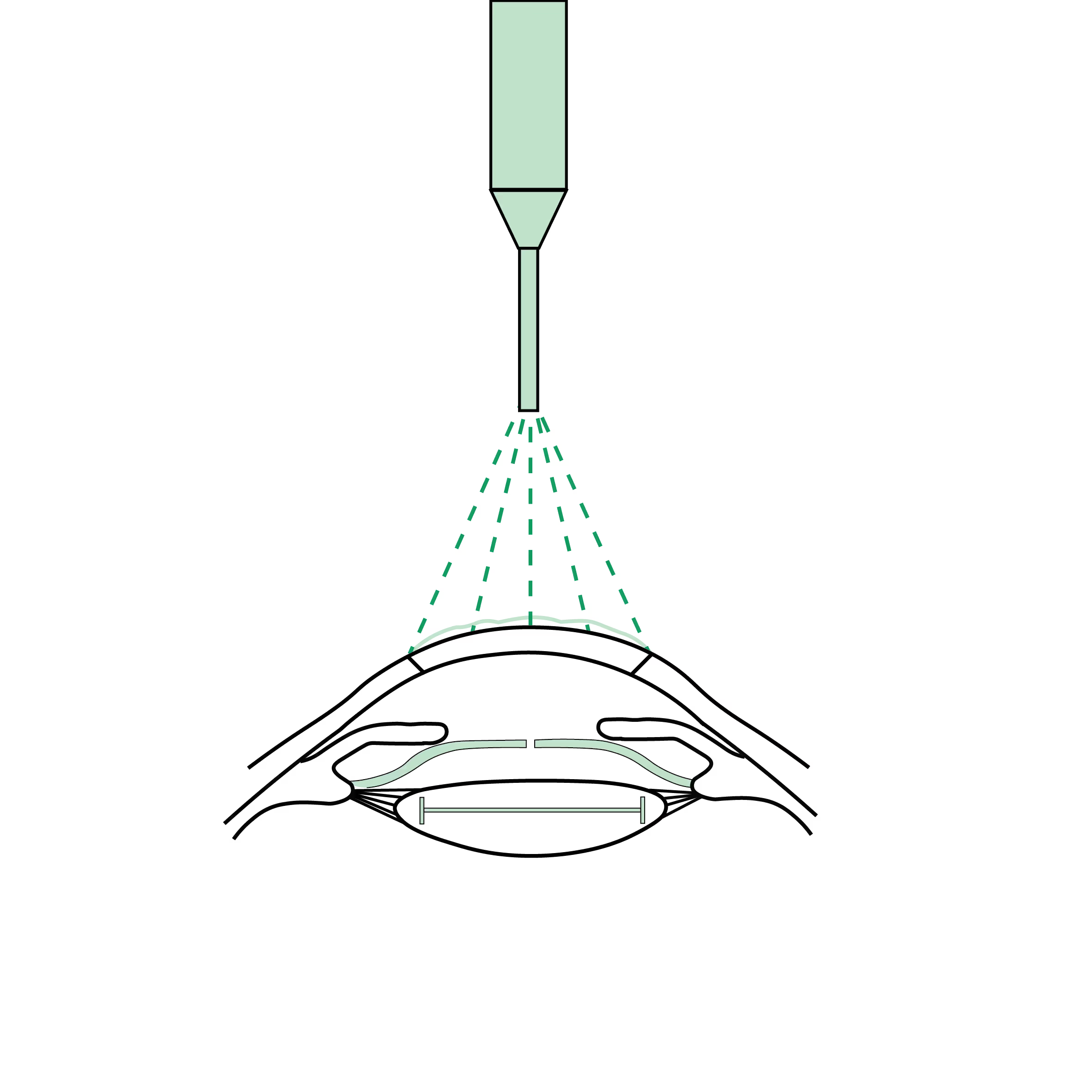
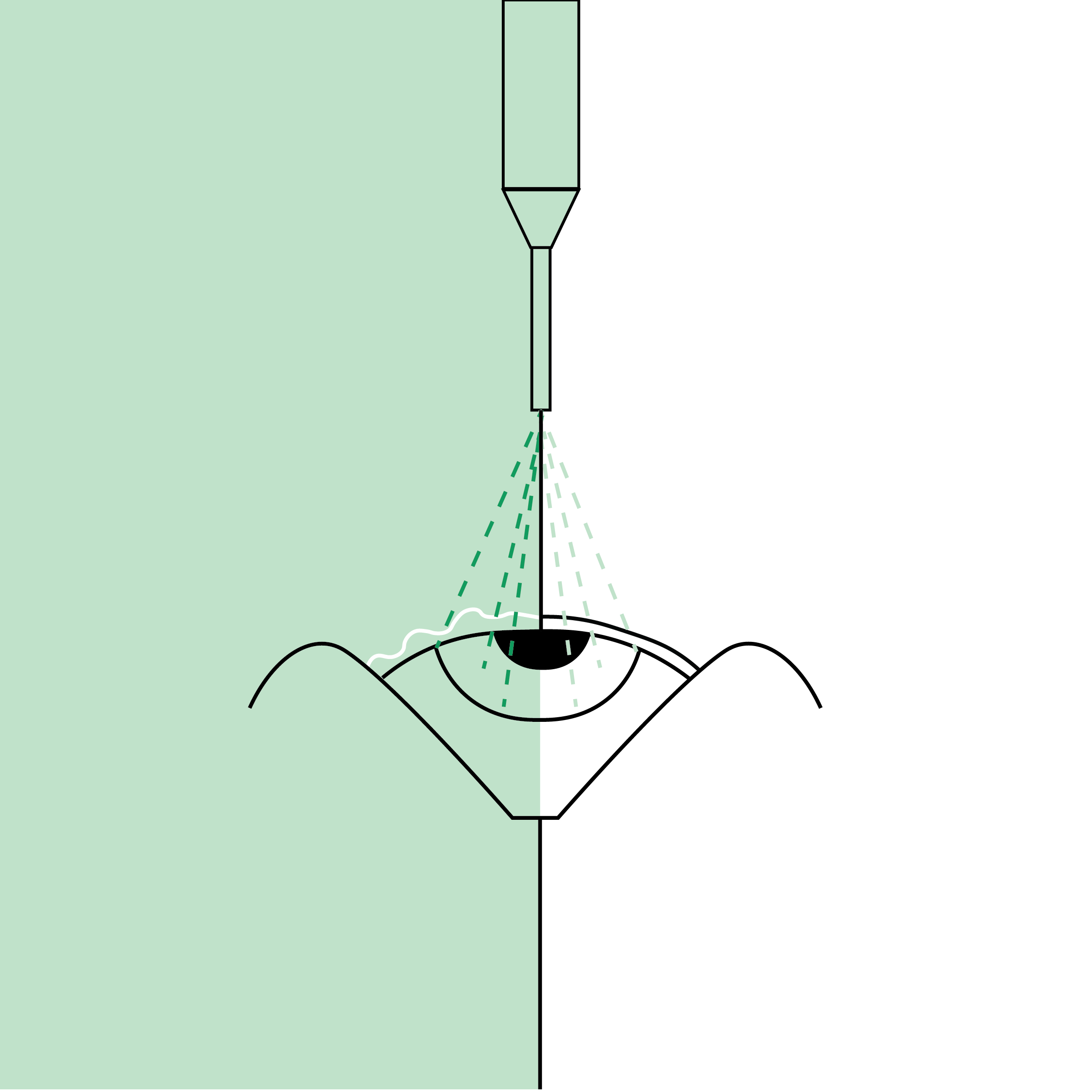
SALK: Superficial Anterior Lamellar Keratoplasty
SALK (Superficial Anterior Lamellar Keratoplasty) is a corneal surgical procedure that replaces only the damaged outer (anterior) layers, while leaving the healthy deep layers intact.
It is typically used to treat superficial opacities or corneal scars that do not extend into the deeper stroma. Because the patient’s own endothelium is preserved, the risk of graft rejection is significantly lower than with a full-thickness transplant.

How does it work?
Learn more about the procedure / equipment
What is SALK?
SALK (Superficial Anterior Lamellar Keratoplasty) is a surgical technique used to treat specific corneal diseases that affect only the outermost layers. It involves removing and replacing the superficial layers of the cornea (the epithelium and the anterior part of the stroma) while preserving the deep layers, including the posterior stroma, Descemet’s membrane and the endothelium.
This technique belongs to the family of lamellar grafts, which aim to replace only the damaged sections of the cornea. This differs from penetrating keratoplasty (PKP), which replaces the entire thickness of the cornea.
What is the procedure?
- Preparing the recipient eye: The superficial layers of the diseased cornea are precisely removed using a surgical trephine or laser, leaving the healthy deep layers intact.
- Preparing the donor cornea: A healthy donor cornea is prepared to match the size and depth of the tissue removed from the patient. Only the anterior portion is used, which significantly limits the risk of rejection.
- Transplantation: The donor graft is positioned onto the recipient’s corneal bed and secured with ultrafine sutures (typically 10-0 nylon), which are approximately ten times thinner than a human hair.
- Postoperative follow-up: Anti-inflammatory treatment, such as steroid eye drops, is prescribed. Regular monitoring ensures the graft adheres correctly and remains free from infectious and rejection episodes.
- Suture removal: Sutures are generally removed 12 to 18 months after surgery, once the graft is stable.
- Visual Rehabilitation: Spectacles or contact lenses may be required once the eye has healed. In some cases, scleral lenses are used to achieve the best possible visual acuity.
- Refractive Surgery: If necessary, laser treatment or intraocular lens implantation can be proposed later to refine the vision and reduce dependence on glasses.
Benefits of SALK
- Endothelial Preservation: By keeping the patient’s own endothelium, the risk of immunological rejection (the primary cause of failure in full-thickness transplants) is drastically reduced.
- Structural Integrity: The eye remains more resistant to trauma compared to a full-thickness graft.
- Sequential Strategy: A deeper transplant can still be performed in the future if the underlying disease progresses.
Possible Risks and Complications
As with all ocular surgeries, SALK carries certain risks:
- Poor graft adhesion (which may require a second intervention).
- Formation of micro-folds or opacities within the graft interface.
- Infection (infectious keratitis).
- Significant or irregular postoperative astigmatism.
- Graft rejection (though this is very rare with this specific technique).
Les différentes types de greffes
Découvrez les kératoplasties (= greffes de cornée)
Frequently asked questions
If you have any further questions, please do not hesitate to contact us!
Linked surgical treatments
Linked conditions
Book a consultation
Swiss Visio Montchoisi
1006 Lausanne, Switzerland