Therapeutic refractive surgery after corneal transplantation
Following a corneal transplant, vision may remain blurred due to discrepancies in corneal curvature or surface irregularities (such as residual astigmatism, myopia, or hypermetropia). Therapeutic refractive surgery enables the correction of these refractive errors through the use of laser technology or intraocular lenses, thereby enhancing visual acuity and reducing dependence on glasses.
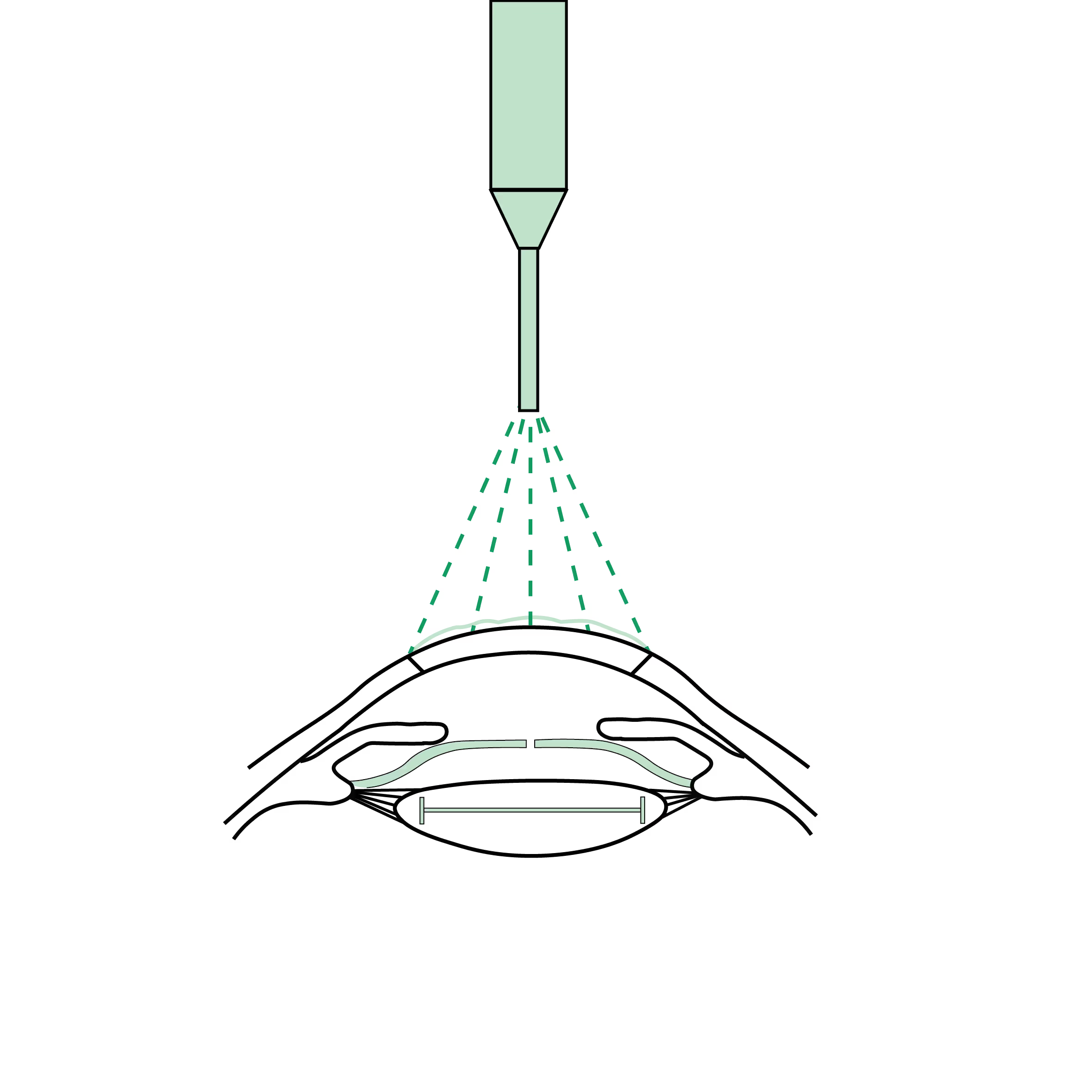
How does it work?
Learn more about the procedure / equipment
What is therapeutic refractive surgery after a corneal transplant?
These procedures are designed to correct refractive errors (myopia, long-sightedness, and astigmatism) that persist following a corneal transplant (Penetrating Keratoplasty [PKP] or Deep Anterior Lamellar Keratoplasty [DALK]).
The primary functional goal is to enhance visual quality and in some instances, also reduce a patient’s dependence on glasses or contact lenses.
This type of surgery is termed "therapeutic" because—unlike standard refractive surgery performed on healthy, "virgin" corneas—its main objective is to manage complex visual irregularities. While the goal is to reduce the need for optical aids, complete independence from glasses can be achieved in some cases.
What are the procedures?
There are several approaches available, depending on the nature of the refractive error and the health of the graft:
1. Laser Surgery (PRK, Trans-PRK, or Custom LASIK)
- Used to correct moderate astigmatism and specific corneal irregularities.
- The laser reshapes the corneal surface to create a more regular profile.
- This requires topography-guided or wavefront-guided (bespoke) mapping to ensure precision.
2. Intraocular Implants (IOL or ICL/IPCL)
- Indicated for high levels of residual ametropia (refractive error) or when laser treatment is contraindicated.
- Cataract Surgery: If a cataract is present, the cloudy lens is replaced with a pseudophakic intraocular lens.
- Phakic Implants: If the natural lens is clear, an implantable contact lens (ICL/IPCL) can be positioned between the iris and the natural lens.
3. Arcuate Keratotomy
- Involves making peripheral incisions to reduce astigmatism induced by the transplant. This can be performed manually or using a femtosecond laser.
Risks and Benefits
Benefits
- Significant improvement in corrected (CDVA)and uncorrected visual acuity (UDVA).
- Reduction of higher-order optical aberrations, particularly in irregular grafts.
- Enhanced daily visual comfort.
- Reduced reliance on glasses or contact lenses.
Risks
- Graft Decompensation: A rare risk where the transplant fails, particularly if surface lasers are too aggressive.
- Induction of new optical irregularities.
- Inflammation or graft rejection triggered by surgical intervention.
- Partial or unstable results that may require further refinement.
The choice of technique is dictated by the type of graft, corneal thickness, the health of the lens, and the dimensions of the anterior chamber.
Indications and Contraindications
Indications (When is it recommended?)
- Significant post-graft astigmatism (typically >3 Dioptres) affecting vision.
- Intolerance to rigid gas permeable (RGP) contact lenses or failure of glasses to provide clarity.
- Anisometropia: A significant difference in prescription between the two eyes causing discomfort.
- Disabling optical aberrations or poor functional vision despite a clear graft.
Contraindications
- An unstable or recent transplant (usually within 12 months of surgery).
- Insufficient corneal thickness.
- Active or recent history of graft rejection.
- Compromised ocular surface (e.g., severe dry eye or chronic inflammation).
- Limited visual potential due to retinal issues.
- Uncontrolled associated conditions such as glaucoma or uveitis.
- Unrealistic visual expectations of the patient.
Les différentes types de greffes
Découvrez les kératoplasties (= greffes de cornée)
Frequently asked questions
If you have any further questions, please do not hesitate to contact us!
Linked surgical treatments
Linked conditions
Book a consultation
Swiss Visio Montchoisi
1006 Lausanne, Switzerland

.avif)
