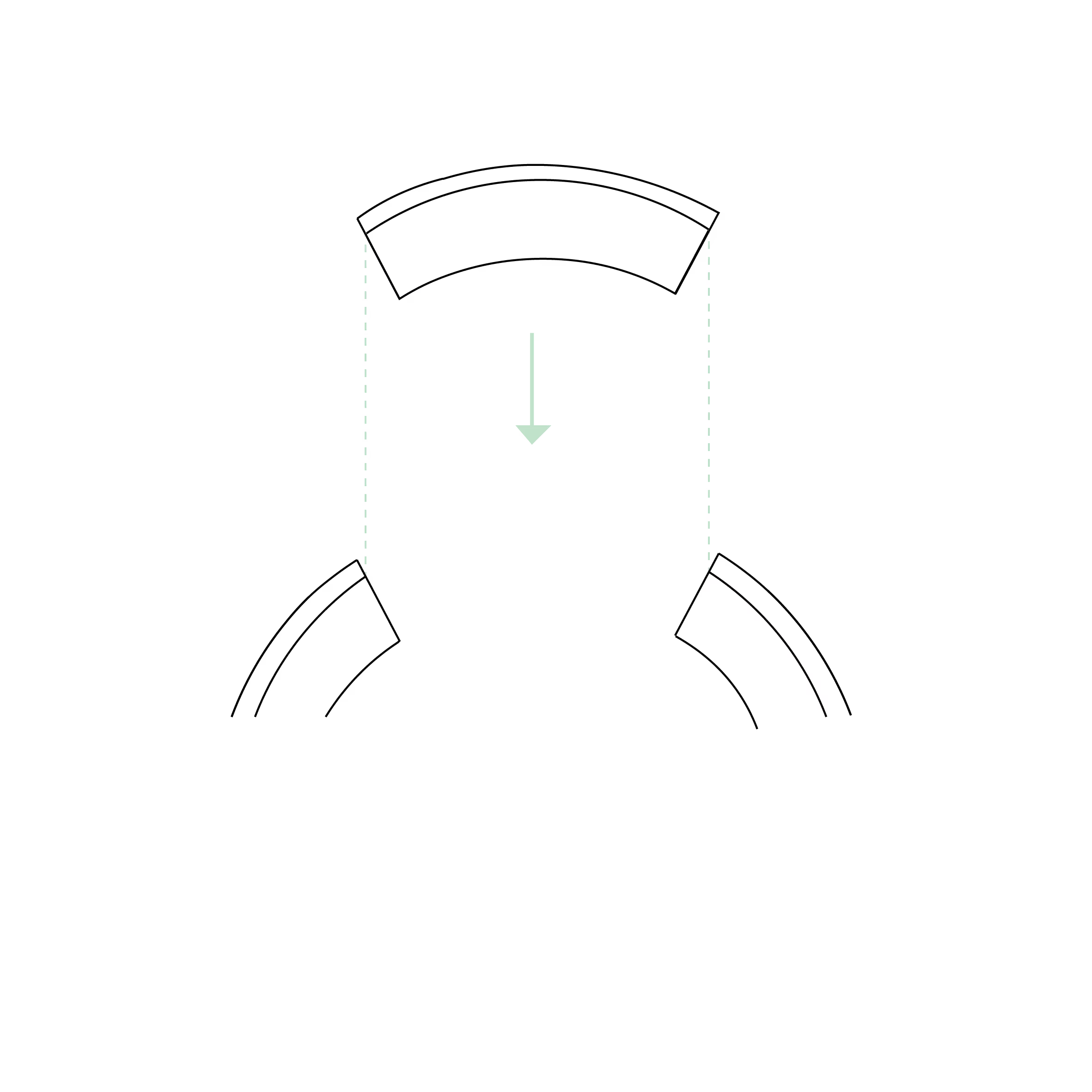
PKP: Penetrating Keratoplasty
PKP (Penetrating Keratoplasty), often referred to as a "full-thickness" graft, is an operation that consists of replacing all layers of the damaged cornea with a healthy cornea from a donor.
This procedure allows the patient to regain clearer vision when their own cornea has become opaque, irregular or compromised. The new donor cornea is secured in place with fine surgical sutures, which are typically ten times thinner than a human hair.

How does it work?
Learn more about the procedure / equipment
What is PKP?
PKP (Penetrating Keratoplasty) is a full-thickness corneal transplant, meaning all layers of the cornea: the epithelium, Bowman’s layer, stroma, Descemet’s membrane and the endothelium are replaced.
The recipient's own limbal stem cells typically restore the surface epithelium. if these cells are unhealthy, a limbal stem cell transplant (such as Auto-SLET) may be required beforehand. PKP is indicated when the cornea is so severely damaged that it compromises vision or the structural integrity of the eye. The procedure uses a healthy donor cornea, usually sourced via a dedicated eye bank.
What is the procedure?
- Preparing the recipient eye: The diseased or scarred cornea is removed using a surgical trephine (a circular precision blade) to cut a disc of tissue.
- Preparing the donor cornea: A matching disc is cut from a healthy donor cornea, often slightly larger than the recipient site to ensure a secure fit.
- Transplantation: The donor graft is precisely positioned over the opening in the recipient's eye.
- Sutures: The graft is secured using ultrafine sutures (either interrupted or continuous stitches), which are significantly thinner than a human hair.
- Postoperative follow-up: Patients must use anti-rejection medication (steroid and sometimes ciclosporin/tacrolimus eye drops) and attend regular check-ups to monitor graft clarity and prevent rejection.
- Suture removal: Sutures are typically removed 12 to 18 months after surgery, once the graft has fully integrated.
- Visual Rehabilitation: Once healed, vision is corrected with spectacles or contact lenses. In some cases, specialised laser surgery or intraocular lenses can be used to reduce dependence on glasses.
What are the risks and benefits?
Benefits
- Significant improvement in visual acuity.
- Restoration of corneal transparency.
- Correction of severe structural deformities.
- "Eye rescue" in cases of corneal perforation.
Risks
- Graft rejection: Symptoms include redness, sudden vision loss, or pain.
- Infection (keratitis or endophthalmitis).
- High and/or irregular post-operative astigmatism (can be corrected with laser surgery or intraocular lenses).
- Recurrence of the original disease (e.g., herpes simplex or certain dystrophies).
Indications and Contraindications
Common indications for PKP include:
- Advanced keratoconus with scarring or extreme thinning.
- Severe corneal scarring (from trauma or infection).
- Inherited corneal dystrophies (e.g., macular or stromal dystrophy).
- Corneal perforation.
Contraindications
- Lack of visual potential: Such as end-stage glaucoma, severe optic neuropathy or macular atrophy.
- Severe dry eye: Extreme keratoconjunctivitis sicca can prevent the graft from healing.
- Uncontrolled inflammation: Active uveitis, cicatricial conjunctivitis or scleritis.
- Poor compliance: Success relies heavily on the patient's ability to adhere to a strict eye-drop regimen and follow-up schedule.
Les différentes types de greffes
Découvrez les kératoplasties (= greffes de cornée)
Frequently asked questions
If you have any further questions, please do not hesitate to contact us!
Linked surgical treatments
Linked conditions
Book a consultation
Swiss Visio Montchoisi
1006 Lausanne, Switzerland