PRK (Photorefractive Keratectomy) laser eye surgery
PRK (PhotoRefractive Keratectomy) is a laser refractive surgery technique used to correct short-sightedness (myopia), long-sightedness (hyperopia), and astigmatism by reshaping the surface of the cornea.
Unlike LASIK, it does not require the creation of a corneal flap. Instead, the epithelium (the thin outer layer of the eye) is temporarily removed to allow the excimer laser to precisely sculpt the underlying corneal tissue. This "surface-based" method is particularly suitable for patients with thin or irregular corneas, offering excellent long-term visual stability.
.avif)
How does it work?
Learn more about the procedure / equipment
What is PRK?
PRK (PhotoRefractive Keratectomy) is a laser vision correction used to treat short-sightedness (myopia), long-sightedness (hyperopia), and astigmatism.
It works by reshaping the surface of the cornea to improve how light focuses on the retina. Unlike LASIK, PRK does not involve the creation of a corneal flap, making it an ideal choice for patients with thin corneas or superficial corneal scars. While the final visual outcomes are comparable to LASIK and SMILE, the initial recovery period is slightly longer.
How does PRK work?
- Preparation: Topical anaesthetic drops are applied to numb the eye. A small, gentle speculum is used to keep the eyelids open, ensuring a stable and precise procedure.
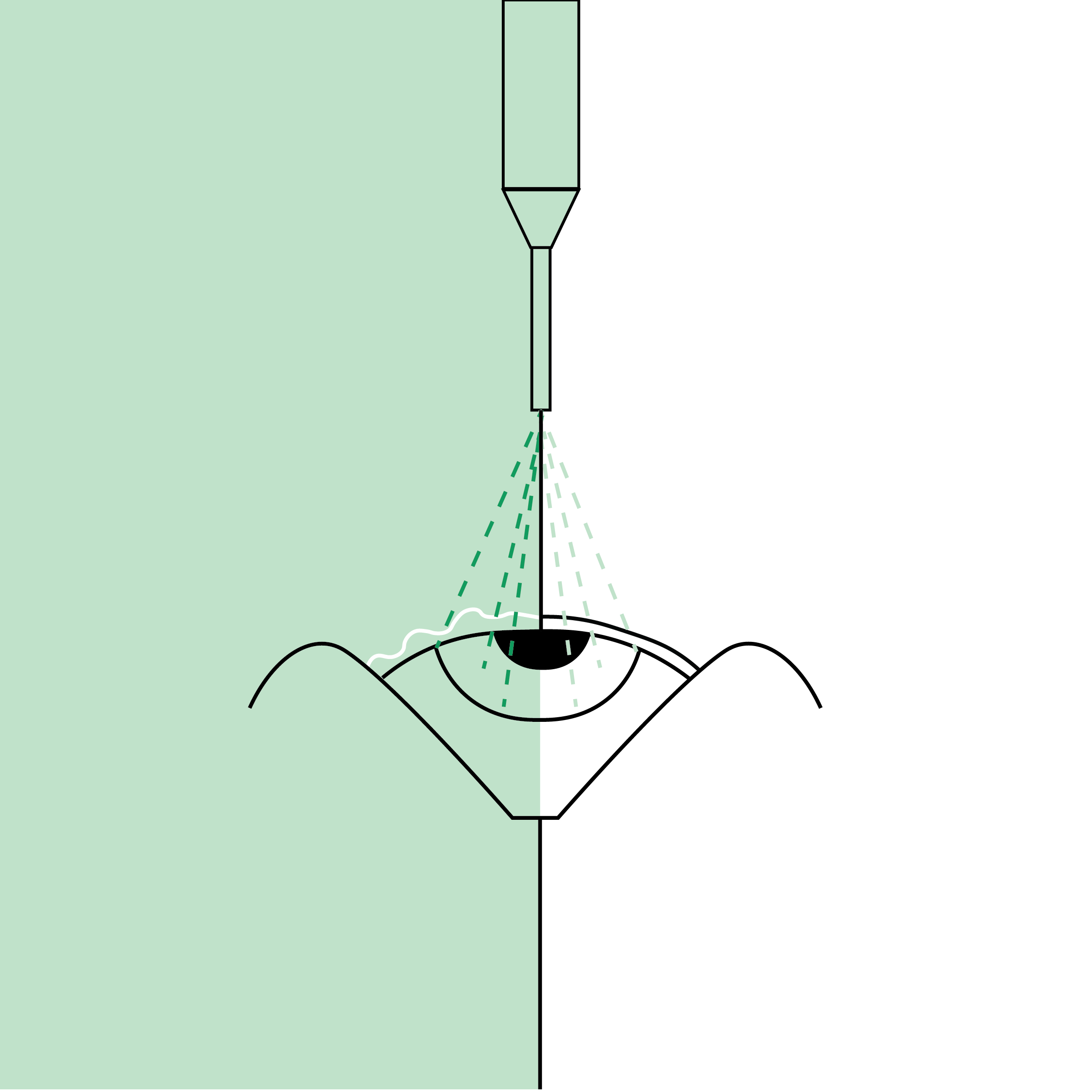
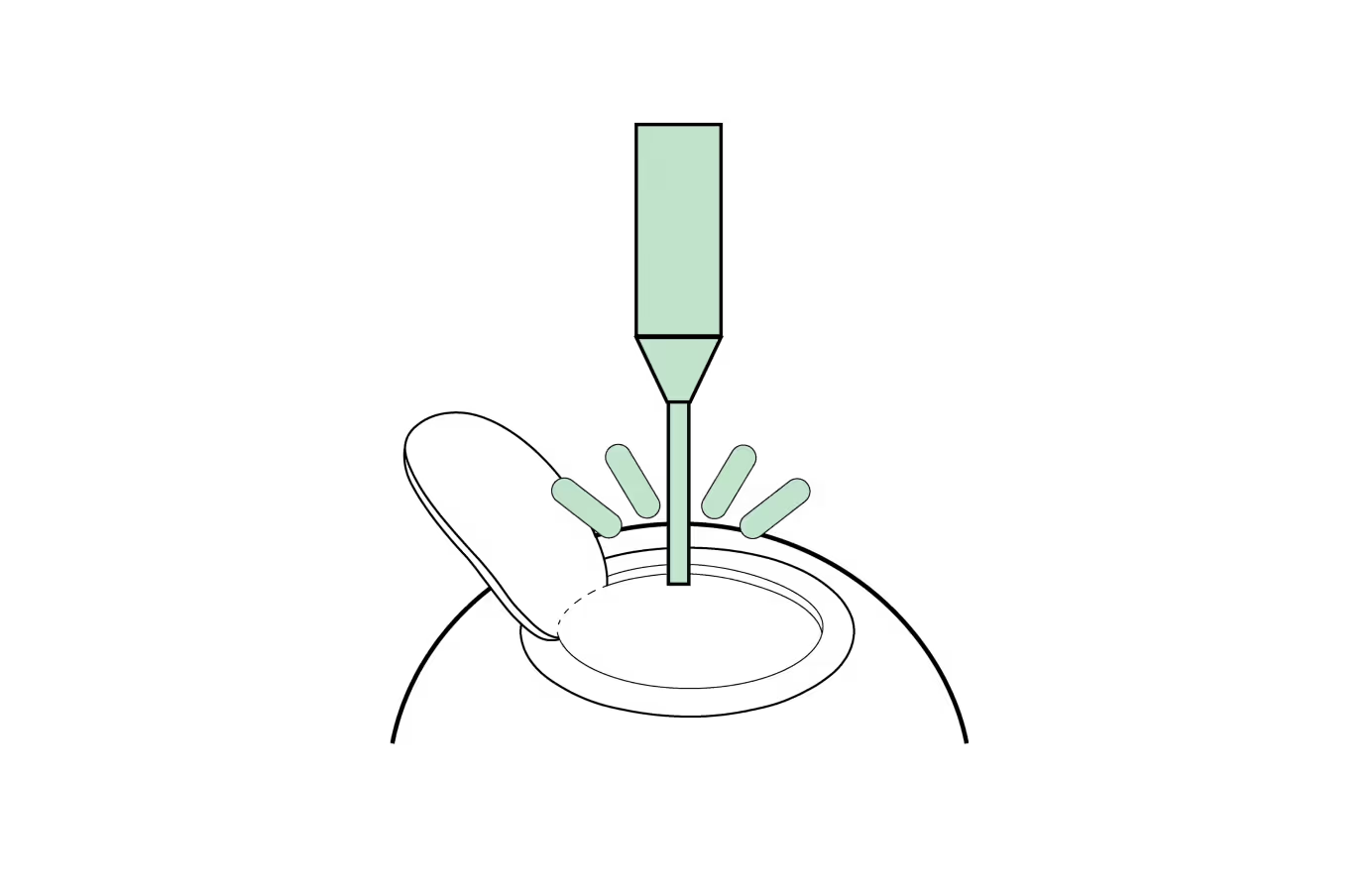
- Epithelium Removal: The thin outer layer of the cornea (the epithelium) is removed to expose the underlying tissue. This can be done mechanically, with a specialized diluted alcohol solution, or directly via the laser (TransPRK).
- Corneal Reshaping: An Excimer laser uses "cold" ultraviolet light to remove microscopic amounts of tissue:
- For short-sightedness: The cornea is flattened.
- For long-sightedness: The cornea is made steeper.
- For astigmatism: The laser smooths the cornea into a more spherical shape.
- Healing: The epithelium regenerates naturally over the following days. A bandage contact lens is placed over the eye to protect the surface, facilitate healing, and minimise discomfort.
- Results: Vision improves progressively. Functional recovery typically takes 1 to 2 weeks, with final stabilization usually achieved within 3 months.
Advantages of PRK
- No Flap Complications: Eliminates risks such as flap displacement, folds (striae), or epithelial ingrowth.
- Suitable for Thin Corneas: The preferred option for patients whose corneas are too thin for LASIK or SMILE.
- Proven Reliability: Final visual results are generally excellent and equal to those of LASIK and SMILE.
- Ideal for Contact Sports: Because there is no flap, SMILE and PRK are recommended for athletes in combat sports or professions with a high risk of ocular trauma.
Who is a suitable candidate?
- Thin or Irregular Corneas: A safe alternative when other laser methods are not recommended.
- Active Lifestyles: Ideal for military personnel, athletes, or those in high-impact occupations.
- Stability: A stable prescription for at least 1–2 years is the primary criterion.
- General Health: Candidates should be in good health, with no uncontrolled autoimmune conditions or significant ocular diseases like advanced cataracts or keratoconus.
- Pregnancy: Candidates should not be pregnant or breastfeeding.
What are the risks of PRK?
PRK is a highly established and safe procedure, though it involves a unique healing process:
- Discomfort: Temporary eye pain or a "gritty" sensation is expected during the first 3–5 days while the epithelium regrows.
- Visual Fluctuations: Blurred vision or fluctuations are normal for several weeks as the new surface smooths over the treatment zone.
- Dry Eye: Temporary dryness is common; it is managed with lubricating drops.
- Corneal Haze: This refers to a slight "cloudiness" or irregular healing of the cornea, particularly in cases of high corrections. This is generally prevented by the application of Mitomycin C (MMC) during surgery. If haze does occur, it may be managed with specific post-operative treatments, such as Losartan eye drops.
- Persistent Epithelial Defect (PED): On rare occasions, the surface layer may take longer than usual to heal. This delayed healing can be treated with specialized interventions, such as insulin eye drops or the application of a healing (bandage) contact lens.
- Infection: Extremely rare (<1 in 10,000) and typically detected early through close post-operative monitoring during the epithelial regeneration phase.
- Corneal Ectasia: An exceptionally rare weakening of the cornea. Proper patient selection and the avoidance of eye rubbing (friction) are essential to prevent this.
Les différentes types de greffes
Découvrez les kératoplasties (= greffes de cornée)
Frequently asked questions
If you have any further questions, please do not hesitate to contact us!
What is PRK?
The PRK (PhotoRefractive Keratectomy) is a form of laser eye surgery used to treat vision problems such as nearsightedness, farsightedness, and astigmatism. This technique involves removing the outer layer of the cornea (epithelium) before reshaping the underlying tissue with a laser.
What is the difference between PRK and LASIK or SMILE?
Unlike LASIK and SMILE, which require the creation of a flap (LASIK) or a lenticule (SMILE) in the cornea, PRK involves temporarily removing the epithelium (the "skin" of the cornea) before laser-reshaping the underlying stroma. It is often recommended for patients with thin, irregular corneas or those not eligible for LASIK or SMILE.
What is the recovery time after PRK?
Recovery after PRK tends to be longer than after LASIK or SMILE. Vision may be blurry for the first few days, and the outer layer of the cornea takes about 3 to 5 days to heal.
Full recovery typically takes between 1 and 3 months.
Linked surgical treatments
Linked conditions
Book a consultation
Swiss Visio Montchoisi
1006 Lausanne, Switzerland

%20au%20laser.avif)

.avif)